An ng-tube, or nasogastric tube, is one type of feeding tube that can be used when a person is unable or unwilling to eat orally. Henry first got an ng-tube shortly after he was born. The doctors immediately recognized his low tone, but did not know the cause, so were worried about possible infections, or other trauma. As he was unable to eat on his own, they inserted an ng-tube.
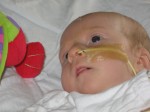
Here is a photo of Henry with his ng-tube, the day after he was born:
Henry has this ng-tube for about 4 days, then we convinced them to remove it and we did a combination of breast-feeding and cup feeding. As Henry grew, he continued to be unable to breast- or bottle-feed successfully, so when Henry was 8 weeks old we made the decision to have an ng-tube reinserted. The cupfeeding was becoming increasingly difficult – with Henry crying and then falling asleep, all the while we’re trying to feed him enough expressed breastmilk (EBM).
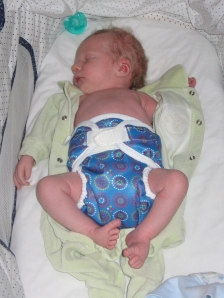
Here’s another photo, when he got his tube back again at about 8 weeks old:
The decision to re-insert his ng-tube may have been one of the hardest decisions Shawn and & I have ever had to make, as it cemented the fact, in our minds, that there was something seriously medically “wrong” with our baby. Up until this point we were banking on the fact that he would outgrow his challenges. Our pediatrician kept hoping that as he put on weight his tone would improve, and we placed our faith in this theory to.
A little about ng-tubes:
Ng-tubes are generally considered temporary feeding tubes, to be used for up to 8 weeks. Having said this, Henry had his for about 8 months, while waiting for his g-tube surgery. Ng-tubes are often used after surgery, until people can eat on their own again, or in people undergoing cancer treatment who are experiencing a lot of nausea. I met one women who needed one when she was pregnant as her morning sickness was so bad she couldn’t keep anything down.
An ng-tube is a thin polyurethane tube, usually with two “ports” at the exterior end and a series of small holes at the interior end. Here’s a picture of the time of ng-tube Henry often had:
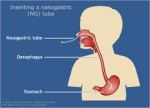
The pink parts are the two ports, this is the end that remains outside the body. The ports are simply opening through which food, water and/or medications are given to a person. This particular tube is yellow and has measurement indicators marked in black. The measurement indicators are helpful to ensure the tube is placed within the stomach correctly. Here is a diagram showing the ng-tube when inserted:
Inserting an ng-tube:
This has got to be one of the worst experiences for Shawn & I. Inserting a tube in an older child or adult can be an uncomfortable, but relatively simple procedure. But inserting it into my screaming child has left me with nightmares. The tube must be inserted through the nose (occasionally through the mouth), and pushed down the throat, passed the vocal cords and into the stomach. All the while ensuring it doesn’t accidentally go into the lungs. If the person is able to sit up, position their head properly and take a drink of liquid- the act of swallowing will help pass the tube down the throat and into the stomach.
However, with Henry all bets are off! From the very beginning he screamed – and rightly so. We would wrap him up in a blanket to give him the feeling of security, and to hold in his arms and legs. Early on we decided that Shawn was the “holder” and I was the “pusher-inner” and our roles remain the same today. Shawn’s job was to hold him as still as possible – especially his head – all the while singing songs, talking, rattling toys… whatever he could do to keep Henry calm. My job was to insert the tube.
Prior to all of this, we would measure to see what length of tube needed to be inserted to reach his stomach. To do this, we measured from the tip of his nose, to the middle of his ear and down to midway between his lower ribcage (the lowest centre point) and his belly button. This was the length of tube needed to ensure the ng-tube would sit at the correct spot inside his tummy. We used a black felt pen to mark a dot on his tube, so that as I was pushing the tube in, I knew when to stop.
So… Shawn’s holding him down and I’ve got the ng-tube ready to go. There’s a small amount of water-based lubricant on this end, to help it slide easier. I push it into and down his nose to the back of his throat. At this point, there is a small amount of resistance and spinning the tube in my fingers often helps it continue. However there was one occasion when I couldn’t get it to go any further and I had to remove it and try again. The tube is flexible, so it if “hits” something it can get stuck. Then… I just keep pushing the tube in until I come to the black dot that we pre-measured. Then Shawn would hold it onto his face and used a syringe to draw out some stomach contents. By using a ph-strip (just like in science class) to test the acid content of the fluid, we knew the tube was in the correct location. If the ph-strip test was good – then we used a bit of tape to adhere the ng-tube and we were done!
Changing the tube:
We changed Henry’s tube each month. At first we didn’t learn how to do it ourselves, and needed to go to the Medical Day Unit (MDU) at Children’s Hospital to have it done. However, it took exactly one week for Henry to pull out his tube the first time, so we quickly decided we had better learn for ourselves! From then we changed it at home, but did go back to the MDU a couple of times when we had problems.
Skin care:
This is a very big deal, especially when using an ng-tube for an extended period of time. The tube is constantly taped to the face, so the skin under the tape can be damaged. For older kids and adults, round tape “dots” can be used which minimize the surface area on the skin. However Henry kept pulling his tube out – so we needed some fancy taping! I’m oddly proud to say that even the nurses at Children’s Hospital used to compliment us on our tape job!
 You can see the difference between the tape in this photo, and the previous one. Just enough tape to keep the tube on, but not a big, wide strip. Plus an added extra below his nose, as this is where he would hook his finger under the tube and pull it out.
You can see the difference between the tape in this photo, and the previous one. Just enough tape to keep the tube on, but not a big, wide strip. Plus an added extra below his nose, as this is where he would hook his finger under the tube and pull it out.
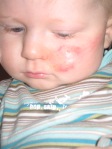
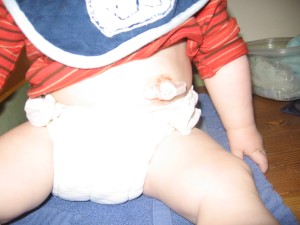
In this photo you can see the redness that develops under the tape. Each time we changed the tube, we switched sides and inserted it into the other nostril. This redness would often take over a week to go away.
Possible Problems:
- nose bleeds – due to the rubbing of the tube. When using a feeding pump (versus gravity or syringe feeding), the tube vibrates and this can cause chaffing.
- aspiration – if the tube is inserted incorrectly, or moves due to a fall or being pulled, the end of the tube could go into the lungs instead of the stomach. Although apparently very rare, and not something we ever experienced, this could cause serious harm.
- sore throat – from the constant presence of a foreign object.
- pulling the tube out – something we experienced repeatedly! Henry seemed to love pulling at the tube, again for obvious reasons… you try having something shoved down your throat and taped to your face! For the first few months, he was in gloves or had socks on his hands 24/7. As he got older, we would take the mitts off during the day, but he always wore them when asleep. Plus he slept on his own little mattress between us in bed for the first year – with Shawn & I both holding onto a hand while sleeping to stop him from rubbing his face. This was our constant battle and one of the reasons we were so glad to get his g-tube.
- clogged tube – plugging up the tube is a problem with any time of tube feeding, but especially ng-tubes. Because they are so thin, it is very important to use lots of water to flush the tube clean. This can be difficult with small infants, like Henry was, because you don’t want to give so much water that they can’t drink enough breastmlk or formula. We did clog his tube a couple of times, but each time were able to get it cleared again without having to change the whole tube.
- public perception – while not really a “problem”, I’ve talked to a number of people who were happy to get rid of the ng-tube so they could go out in public for once and not have people ask what’s “wrong” with their child. And I agree! Even really caring, thoughtful people who in no way want to be rude, stare at a baby with an ng-tube. And it gets tiring… So as horrible as it may sound to someone who’s never experienced it, I was glad to get rid of Henry’s tube… I was glad to stop pretending to myself that people weren’t staring… and I was glad to stop having to explain myself… because not everyone is actually that nice…
Ng-tubes and Homemade Blended Formulas
Because the main purpose of my blog is our experiences with homemade blended foods, I thought I’d include a bit about how ng-tubes work with blenderized diets. We never tried homemade foods with Henry’s ng-tube. Well, actually… I guess we did – after all, expressed breast milk (EBM) is the ultimate “homemade” food! At the time he had his ng-tube, Henry was getting exclusively EBM. It passed through the tube just fine, and as long as we flushed enough water down the tube afterwards, it didn’t clog.
According to the Homemade Blended Formula Handbook (still my favourite book!), it is possible to augment a commercial formula by adding in some blended whole foods. But it would be virtually impossible to use an entirely homemade formula – the tube is too thin. The food would need to be diluted to such a degree it would be impossible to get enough nutrition. But it’s definitely possible to add in some blended fruits or veggies!
So… that’s my thoughts on ng-tubes. Both Shawn & I are very thankful the technology exists to allow us to feed our baby. Apparently it was not that long ago that people with ng-tubes had to stay in the hospital – there was no system in place for tube feeding at home. It was likely one of the most stressful times in our lives – both as individuals and as a couple – but we persevered and made it through.
We struggled for months with the decision as to whether Henry should have the surgery for a g-tube, but we are most definitely happier now that it’s done… and so is Henry :).
Cheers, Shelley